Physicians Practice
March 2007

The Infertility Center of St. Louis at St. Luke’s Hospital has a national reputation for excellence primarily because they have brought innovation and advancement to the field of infertility treatment. Led by Sherman Silber, MD, the Infertility Center of St. Louis has pioneered a number of methods to combat infertility that have become new standards in the field, and the Center doesn’t shy away from taking on patients that have often been told that there is no hope that they will ever become pregnant.

of the Infertility Center of
St. Louis at St. Luke’s Hospital
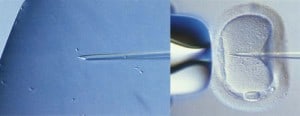
In 2005, Child Magazine recognized the Infertility Center of St. Louis at St. Luke’s Hospital as one of the Top 5 infertility centers in the United States, and the number one infertility center in the entire midwest. Some of the innovative procedures performed at the Center include the first successful microscopic vasectomy reversal, intra-cytoplasmic sperm injection (ICSI), the world’s first ovary transplant surgery and a new method first developed by researchers in Japan called minimal stimulation. The first of these new treatments deals specifically with men who have been told that because of their low (often considered zero) sperm count there is no possible chance of making their partners pregnant. These men are often candidates for the intra-cytoplasmic sperm injection (ICSI) technique. This procedure was developed and perfected through a partnership with the Brussels University and the Infertility Center of St. Louis. Sperm is retrieved through a microsurgical technique [see technical video] directly from the testicle. Then, sperm that is found to be in good condition is injected, one at a time, directly into the egg of the female partner. The fertilization rate per egg using ICSI is about 70 percent despite often poor sperm quality, and the fertilization rate per infertile couple is over 99 percent if the female partner’s eggs are adequate. The success rate of ICSI is equal to that of men with normal sperm count.
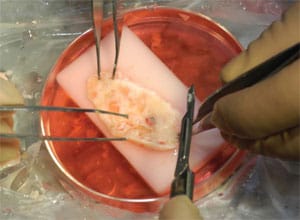
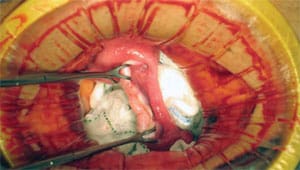
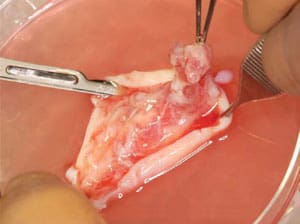
Perhaps the most well known infertility treatment recently developed by Dr. Silber and performed by Dr. Silber and his colleagues at St. Luke’s Hospital is the ovary transplant surgery. In April 2004, Dr. Silber, along with David Levine, MD, an obstetrician on staff at St. Luke’s who is board certified in both Gynecology and Urogynecology, and Jorge Pineda, MD, board certified in Obstetrics and Gynecology and Reproductive Endocrinology, transplanted an ovary from a healthy, fertile 24 year-old female into her infertile identical twin sister [see video]. The infertile twin had undergone menopause at the age of 14 because of a genetic defect. In this surgery, the sterile twin received ovarian cortical tissue from her sister by means of a minilaparotomy. Three months after the procedure, the recipient’s menstrual cycles resumed and ovary function became normal. During her second menstrual cycle, she Injection of the sperm into the egg. During the ICSI procedure, the sperm is captured and immobilized. During an ovary transplant, healthy tissue is extracted from the donor ovary. The donor ovary is prepared for transplantation. became pregnant. She and her husband became parents of a healthy baby girl [see video] in June 2005, and the case was published in the New England Journal of Medicine [PDF file] on July 7, 2005. Since this initial surgery, the Infertility Center of St. Louis has been contacted by a number of female identical twins with one fertile and one infertile sister. Dr. Silber and Dr. Pineda have performed four additional ovary transplant procedures at St. Luke’s Hospital. The second case has also resulted in a healthy pregnancy, and all five cases have been successful with normal menstruation and ovulation, the last three too early to have produced a pregnancy.
Another new procedure practiced at the Infertility Center of St. Louis is the minimal stimulation procedure. This method can be considered ideal for couples in cases in which the female’s eggs are considered poor quality. Using the traditional drug Clomid through day 12 of a menstrual cycle increases estrogen while the follicles are developing but prevents ovulation. This results in great quality of eggs and embryos, but temporarily thins the uterine lining in that cycle, preventing the embryo from attaching. The eggs are then frozen through a new process called vitrification – at 20,000 degrees centigrade per second – which prevents the formation of ice crystals inside the eggs [see video]. Then, the eggs are transferred one at a time back to the female patient in subsequent natural cycles. Minimal stimulation has comparable pregnancy rates as traditional in vitro stimulation with less need for monitoring, greater patient comfort due to the lower levels of hormones required, and lower cost. In each and every couple who comes to the Infertility Center of St. Louis at St. Luke’s Hospital, there is hope for one day becoming biological parents. And in each case, the best possible course of treatment is determined and often the infertile couple’s hopes and dreams become realities.
The donor ovary is prepared for transplantation. Healthy ovarian tissue is implanted in the recipient completing the ovary tissue transplant.