Doctor from St. Luke’s Hospital will be the first to try the live transplant in the United States to help infertile woman.
Front Page – St. Louis Post Dispatch, April 21, 2004
by Tina Hesman of the Post-Dispatch
A St. Louis fertility specialist is set to perform a transplant today that may be the ultimate “gift of life.”
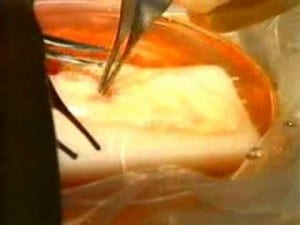
Dr. Sherman J. Silber, director of the Infertility Center of St. Louis at St. Luke’s Hospital, will transplant an ovary from an Alabama woman to her infertile identical twin. It is the first time such a transplant has been tried in the United States, Silber said.
The sisters, Melanie Morgan and Stephanie Yerber, 24, share the same genetic makeup, with the possible exception of one or more genes controlling the start of menopause, Silber said. Both twins entered puberty normally, but Yerber began to go through menopause at age 13 while her sister stayed fertile.
Collaborators at the Paternity Testing Corp. in Columbia and at the MIT Whitehead Institute will examine the sisters’ DNA for small differences that could be linked to reproduction. The analysis could lead to new insight on the genetic cause of menopause, Silber said.
Silber transplanted a testicle from one twin into his brother in 1977. The formerly infertile brother now has four children. Several other testicular transplants in the 1970s convinced Silber that he could do the same for female twins. But such cases arise rarely, he said.
The procedure is a last-ditch attempt for Yerber to become pregnant. Morgan, who has three children of her own, donated eggs for in vitro fertilization attempts several times. None of those tries resulted in pregnancy.

So the sisters sought out Silber and asked him if he could transplant an ovary from Morgan into her infertile sister. The doctor agreed to try the unusual surgery. Because the women are twins, Yerber will not need to take immune-suppressing drugs. Even closely matched siblings would usually require the drugs to stop the recipient’s body from rejecting the transplanted tissue, he said.
Ovarian transplants are not completely new. Scientists have been working for years to learn how to freeze eggs and preserve a woman’s fertility – so far unsuccessfully in humans.
Scientists at the Oregon Health & Science University reported last month in the journal Nature that a baby rhesus monkey was born after a successful ovarian transplant of the mother’s own tissue to another part of her body.
That technique holds hope for women who face chemotherapy and would like to freeze their ovaries. The organs are usually transplanted in the arm, near the kidneys or in other parts of the body. As a result, doctors must harvest eggs from the transplanted ovary and fertilize them in the laboratory before transferring the embryo to the mother’s womb.
No babies have been born from that process. But the technology has advanced enough so that doctors can coax frozen, thawed, transplanted ovaries to produce hormones again.
If Morgan’s transplanted ovary functions properly, it could produce significant health benefits for Yerber by eliminating the need for hormone replacement therapy, Silber said. Hormone therapy has been linked to an increased risk of stroke, heart attack, breast cancer and Alzheimer’s disease in women who take the drugs after menopause.
Silber will transplant the ovary in place of one of Yerber’s own defunct ovaries. In about three months, Silber expects the ovary to start normal hormone cycles and produce mature eggs, ones that are ripe for pregnancy.
“The whole idea of this is a natural pregnancy,” he said.
Front Page – St. Louis Post Dispatch
April 21, 2004