How Does the Biological Clock Work?
Beating Your Biological Clock
Written by: Sherman J. Silber
Click Here to download Beating Your Biological Clock in PDF format.

How Many Eggs Does a Woman Have?
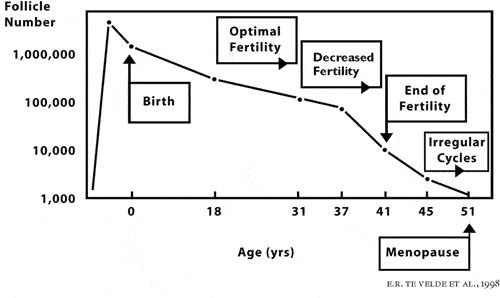
Women are born with all the eggs they are ever going to have, and they don’t make any new eggs during their lifetime. Women are born with approximately two million eggs in their ovaries, but about eleven thousand of them die every month prior to puberty.
Egg Count by Age
As a teenager, a woman has only three hundred thousand to four hundred thousand remaining eggs, and from that point on, approximately one thousand eggs are destined to die each month.
This phenomenon is completely independent of any hormone production, birth control pills, pregnancies, nutritional supplements, or even health or lifestyle. Nothing stops this inexorable death of approximately one thousand eggs every month regardless of ovulation, ovarian inhibition, or stimulation.
Whenever the woman runs out of her supply of eggs, the ovaries cease to make estrogen, and she goes through menopause. Despite a lot of journalistic hype, there is no similar phenomenon in men. Men continue to make sperm and testosterone at virtually the same rates, with only a very modest diminution as they age.
How Many eggs Does a Woman Have at 40?
Many population studies have demonstrated over several decades that the average fertile woman becomes infertile by age forty or earlier, and undergoes menopause by age fifty. The mean age of the end of female fertility (according to all the early population studies of fertile women) precedes menopause by about ten to thirteen years. The end of fertility for an otherwise normal, fertile woman, and the age of the onset of menopause, correlates strictly with the decline in the number of eggs remaining in her ovary.
The average female life expectancy in the Western world is currently about eighty-four, whereas in 1900, the average life expectancy was fifty, and in 1850, it was only forty-two years of age.
Meanwhile, the average age at which young girls start menstruating in the modern world has decreased from age thirteen or fourteen to age ten or eleven. Neither the overall life expectancy, nor the age of menarche (the beginning of menstruation) has any effect on the average age of menopause. In fact, the average age of menopause in almost every population studied over any period of time and in any era has remained constant at around fifty.
Although some women go through menopause in their twenties (because of POF, i.e., premature ovarian failure) and some go into menopause in their late fifties, the timing does not appear to depend upon any specific element in their lives other than the number of eggs with which they were endowed at birth.
It is this wide variation in endowment of eggs from woman to woman that will determine whether you will lose your fertility early (late twenties or early thirties), or whether you’ll be one of the lucky women who is able to have children into her mid- or even late forties.
To recap, the average woman will have three hundred thousand to four hundred thousand eggs at the time of puberty. An average of one thousand will die every month, and only one of those thousand every month is destined to ovulate.
By age thirty-seven, the average woman will be down to only about twenty-five thousand remaining eggs. When only twenty-five thousand eggs remain in the ovaries, menopause will occur in approximately thirteen years.
At What Age Are Women Likely to Become Infertile?
Thus, the average woman begins to become infertile by age thirty-seven or earlier, when her ovarian reserve goes down to about twenty-five thousand eggs, and at age fifty, she will go through menopause. But there are wide variations from this average. What you need to know, in order to plan your entire life, is where you fit on that curve (see fig. 3).
Antral Follicles and Your Ovarian Reserve
To understand how an antral follicle count [see video] ultrasound can tell you where you are on your biological clock, remember that approximately thirty to thirty-five eggs die every day. That is where the number of one thousand per month comes from. They die only because they have initiated their emergence from the resting pool of eggs and have begun their long, three-month development toward becoming an egg that is capable of ovulation.
Only one every month, out of the one thousand that tried, will ever make it. In other words, every day thirty or so eggs that are otherwise safely resting in your ovary, protected from the ravages of age by being in a quiescent phase, emerge by some signal that scientists still don’t understand into a very long (approximately three-month) developmental process that is completely dissociated from your menstrual cycle or your ovulatory cycle.
Once that three-month growth has reached the antral stage, when the follicles finally become sensitive to the hormones of your monthly menstrual cycle, they will rapidly die and disappear if they are not rescued by FSH. Here is how it happens:
Each egg in your ovaries is enclosed within a resting follicle. Every day, thirty to thirty-five of these resting follicles begin their eighty-five days of development toward eventually trying to ovulate.
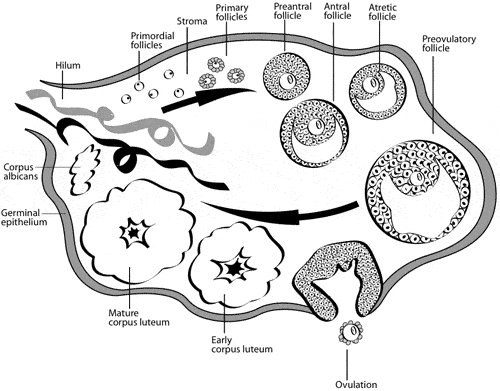
At any time, a view into your ovary reveals follicles (with their enclosed eggs) in every stage of resting or growing (see fig. 4). There are early primordial, or resting, follicles; there are somewhat larger primary follicles; there are larger pre-antral follicles (which are beginning to form a fluid-filled space); and there are antral follicles, which are just becoming visible under ultrasound at a size of approximately one to two millimeters in diameter. In addition, at midcycle, on day fourteen, there is normally a dominant pre-ovulatory follicle. After ovulation, that follicle becomes a corpus luteum, which begins to secrete progesterone.
It is often erroneously thought that just one follicle develops every month, during the first two weeks of the cycle, ultimately culminating in a large, twenty-millimeter follicle from which the egg is ovulated at approximately day fourteen (in a typical twenty-eight-day ovulatory menstrual cycle).
Development of this single, dominant follicle every month with its increasing production of estrogen, and the entire regulation of the monthly cycle via the pituitary hormones of FSH and LH, only gives a tiny part of the picture; it only shows what is happening to one egg in an ovary that contains, in a fertile young woman, as many as 200,000 eggs.
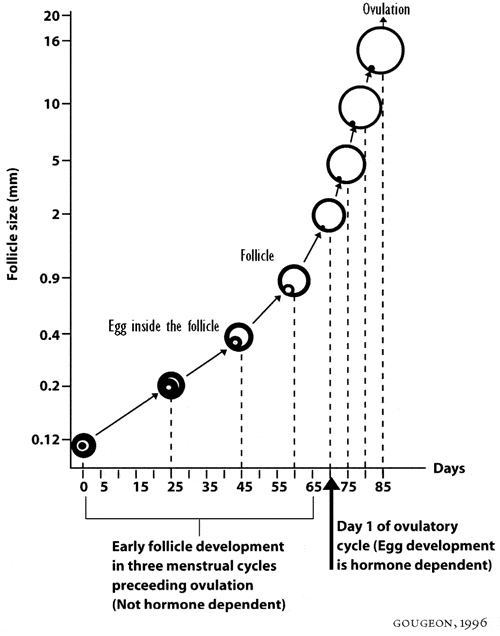
That one egg that was destined to ovulate, developed as the single dominant follicle out of the thirty or so much smaller pre-antral and antral follicles, which had been developing in the ovary for as long as seventy days prior to the beginning of the current twenty-eight day menstrual cycle (see fig. 5).
Most of the ovaries’ 300,000 to 400,000 follicles are quiescent and doing nothing during any given month, but out of that primordial pool a certain number (an average of thirty to forty) will begin to develop each day.
By approximately seventy days of development, these follicles will have grown to approximately two millimeters in size, and at that size they are readily visible with modern, high-quality ultrasound scanning.
During the first seventy days of a follicle’s development, it is completely independent of any hormonal influence. FSH and the monthly hormonal cycle have no influence yet. Sometime between 0.2 millimeters and 2 millimeters in size, these so-called antral follicles begin to become sensitive to stimulation by FSH from the pituitary gland. Prior to the time when these tiny follicles finally become ready to enter the current menstrual / ovulatory cycle, they are completely unaffected by whatever hormonal events have been taking place in the previous cycles.
As previously stated, the number of follicles leaving the resting pool (destined to become either the lucky egg that is ovulated, or the unlucky ones that undergo atresia, i.e., cell death) may average about thirty per day, or one thousand per month, and that number is related to the age of the woman, and to her declining fertility.
Thus, when a woman is only twenty years of age, an average of thirty-seven follicles per day leave the resting stage. When she is thirty-five years of age, an average of ten follicles per day leave the resting stage, and when she is forty-five years of age, an average of two follicles per day leave the resting stage.
This means that the number of follicles per day that begin to become antral, and thereby capable of rescue from death by FSH stimulation, is inversely related to the age of the woman. The younger the woman and the larger the total number of eggs in her ovaries, the greater the number of eggs in any given month, or any given day, that will leave the resting phase and develop into antral follicles (of which only one per month is destined to ovulate; all the others will die).
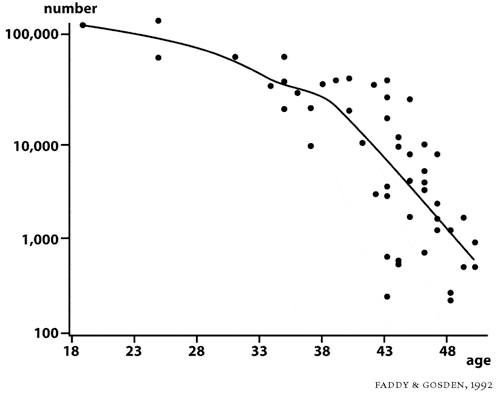
So the number of egg-containing follicles remaining in the ovary undergoes a steady decline from an average of 400,000 eggs at age eighteen to an average of 25,000 eggs by age thirty-seven. After age thirtyseven or thirty-eight, there is then a very dramatic acceleration of the monthly decline of remaining eggs.
Not only is your egg / follicle pool already down because of a steady decline over the previous twenty years, but the rate of the decline after age thirty-seven becomes even steeper than in prior years (see fig. 6). The number of follicles per day that leave this resting pool and begin the three-month developmental path toward being available for future ovulation diminishes dramatically in direct proportion to the number of eggs that are left in the ovary.
Egg Count Test – Antral Follicle Count
When the antral follicle first becomes large enough (one to two millimeters) to be visible on ultrasound, it then also becomes susceptible to hormonal stimulation, and the number of visible antral follicles is directly proportional to ovarian reserve. Therefore, the antral follicle count as determined by ultrasound will give you an accurate read on how many eggs are left in your ovaries.
The antral follicle count also tells you the number of eggs that can be retrieved in an ovulatory stimulation cycle for IVF. To understand this, we will quickly review the normal menstrual cycle with the ovulation of a single egg and explain what happens when we give FSH injections to stimulate multiple follicle development for an IVF cycle.
Remember that the number of eggs we are able to retrieve in an IVF cycle, regardless of age, is the most important determinant of your likelihood of pregnancy; it is also the most important determinant of any age-related decline in your natural fertility.
Emergence of the Dominant Single Follicle During a Normal Ovulatory Monthly Cycle
At the time of your menses (menstruation), as a result of the rapid fall in estradiol (estrogen) and progesterone secretion from the ovulated follicle of the previous month, the uterus sheds the lining that had built up during that month in preparation for pregnancy (see fig. 2).
This sudden drop in estrogen causes the FSH secreted from the pituitary gland to rise dramatically around day twenty-six of the previous twenty-eightday cycle. So, two days later, on day one of your menstruation (the beginning of your next cycle), this elevated FSH stimulates only the development of follicles that had left the resting pool 70 days earlier, and that are now antral.
As these antral follicles grow in response to FSH, they secrete estrogen and inhibin B, which in turn suppress further the pituitary secretion of FSH. Thus, as the antral follicles become more mature (by day six), the FSH begins to decline. If these antral follicles were not rescued by the increased FSH level on day one of the menstrual cycle, when they have finally reached the antral size, they would die immediately.
A competitive struggle then ensues between all of these approximately thirty antral follicles to see which one will become the “lead follicle” that will ovulate on day fourteen. The antral follicle that is most sensitive to FSH in the first few days of your cycle becomes even more sensitized to FSH, and thus gains the lead over all the other follicles (which die off because of lower and lower levels of FSH).
Once the dominant follicle gains the lead, it will never relinquish it, because it requires less FSH than the others to get the same degree of stimulation. Because FSH continually declines toward the middle of your cycle just prior to your ovulation, all the other antral follicles that month (which have finally become hormone dependent after almost three months of non-hormone-related growth) will die.
When they reach this stage of development, the follicles are completely dependent on FSH for survival. Once the estrogen production exponentially peaks, around day twelve or thirteen, it stimulates a dramatic rise in LH from the pituitary gland, and that rise in LH is what prepares the one remaining follicle for ovulation.
In preparation for IVF, FSH injections are given in the early part of the cycle so that the FSH level never declines, as it would normally.
This sustained elevation of FSH, which is all that the administration of ovulatory stimulation hormones amounts to, sustains almost all of the thirty or so antral follicles so that no single follicle can gain dominance over the others.
Therefore, the number of eggs retrieved in a hormonal stimulation cycle for IVF is directly reflective of your antral follicle count, and your antral follicle count is directly reflective of your total remaining number of eggs.


