Mini IVF Yields Better Quality Eggs
Dr. Silber Explains
Mini-IVF was first developed by the Kato Ladies Clinic in Japan and then perfected and popularized by us at St. Luke’s Hospital in St. Louis. It takes advantage of your own natural FSH elevation with an ingeniously simple protocol that strives for smaller numbers of better quality eggs. Instead of massive doses of expensive hormones to try to blast out a few poor quality eggs, it more naturally teases out of even older ovaries their best quality eggs with a carefully devised protocol of minimal stimulation. There are no symptoms of huge hormonal swings or hyperstimulation. It is easier on the patient and much cheaper than conventional IVF.
Our approach to minimal stimulation (Mini-IVF) allows us to retrieve just as many (or few) eggs from the woman as more expensive, conventional stimulation protocols, but better quality eggs and at a lower cost with essentially no complications. We can freeze the embryos with impunity (our freezing does no damage to the embryo whatsoever) and then transfer them back to you in a later cycle when the uterine lining is more perfectly synchronized to the stage of embryo development than during a stimulated cycle. This all adds up to better success rates in even the most challenging cases, and at far less cost and aggravation for the patient.
Dr. Silber Explains Fertilization Rates
Mini-IVF is tricky to perform well and many centers are not up to it. It is easier for the patient and more difficult for the doctor. There is no margin for error. There are several reasons for the success we have with these much lower cost mini-IVF techniques.
The success of this approach depends not only on a novel endocrine stimulation protocol, but also upon a flawless method of embryo freezing such as our vitrification system, and the highest level laboratory air purification system to give the eggs especially from older women the best possible environment in which to develop.
With our mini-IVF approach of storing up vitrified embryos month by month in older women, we have remarkable pregnancy rate even in women over 42-years of age of over 50%. But it takes a great deal of patience on the part of the patient to retrieve just a few eggs at a time every month until enough embryos are banked to warrant thawing and transfer. In addition, the endocrinology of mini-IVF is very innovative and requires close attention to each individual patient to avoid premature ovulation.
Each Patient Has Their Own Incubator
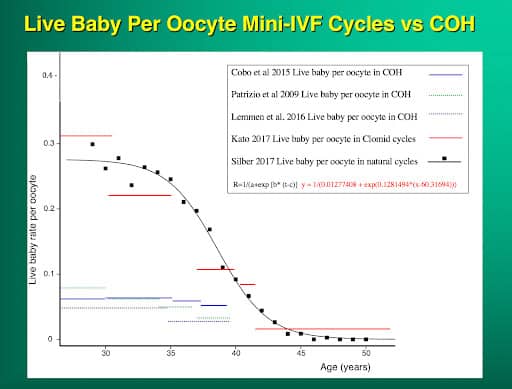
Take a look at this graph showing live baby rate per egg with Mini-IVF compared to conventional ovarian stimulation. The baby rate per egg is 4 to 5 times greater with Mini-IVF at any given age. Even at older ages, the baby rate per egg is four to five times higher than with high dose hyperstimulation. Please note, we use now use Mini-IVF for all patients, good prognosis and poor because at any age the baby rate per egg is 4-5 times higher.
Is Mini-IVF Always Used ?
No, it is most useful for older women and women with low ovarian reserve. There are still many patients who are happy with conventional stimulation. However many of these women also prefer mini-IVF because of the lower cost and the lack of any risk of hyperstimulating syndrome. Even younger patients prefer mini-ivf because of much lower cost, no hyperstimulation syndrome risk, and frankly, better results.
Cost
Better results are the ultimate method for cost savings but also our charges remain very low to reasonable because we don’t try to empty your wallet with unnecessary testing and low yield procedures prior to your IVF.
Technical Scientific Talks by Dr. Silber
Process
Mini-IVF is designed to recruit only a few (but high quality) eggs, thus avoiding the risks of hyperstimulation, reducing the number of injections and dramatically reducing the cost of medications. However quite remarkably, we are now finding that with the lower dose mini-ivf protocol, we are actually getting more eggs as well as better quality eggs. In many patients who had very poor quality embryos with conventional IVF stimulation protocols, mini-IVF dramatically improved their embryo quality and resulted in pregnancy in otherwise “hopeless cases”. This approach is not just a simple-minded reduction in hormonal stimulation. It is an ingeniously conceived and completely different stimulation protocol that saves the patient much of the complexity and cost associated with more conventional IVF protocols. Here is how it works:
On day 3 of the menstrual cycle, you start on a low dose of Clomid (50mgs), but you do not stop the Clomid in five days, as is usually the custom. You keep taking the Clomid until ultrasound monitoring shows the follicles to be ready for ovulation. A very low “booster” dose of gonadotropin (just 150iu of FSH) is added on days 8, 10, and 12. Clomid not only stimulates your own pituitary to release FSH naturally (by blocking estrogen’s suppressing effect), but when you continue the Clomid (a new approach), it blocks estrogen’s stimulation of LH release, and also usually prevents premature ovulation. Thus, with this simple change in protocol, the old-fashioned, inexpensive Clomid is able to stimulate the development of great-quality eggs for IVF.
Another advantage of this protocol is that you do not have to go on Lupron first to suppress the pituitary. Staying on Clomid blocks estrogen from stimulating your pituitary to release LH, and this added effect of Clomid will prevent premature ovulation. This means that you can be induced to ovulate with just a simple injection or nasal sniff of Lupron. This causes a more natural LH surge and avoids the defect caused by the prolonged effect of an HCG trigger. This leads to more “natural” maturation of the eggs.
The next step is to recognize that Clomid has a temporarily negative effect on the uterus (because it blocks estrogen’s support of the developing endometrial lining). That is one reason why results in the past have been so poor with the use of Clomid for ovarian stimulation. The embryos are less likely to implant in such an endometrium. But that problem is now easily solved by using the Japanese protocol for embryo freezing, “vitrification” which I discuss elsewhere. We can now freeze the embryos almost with impunity using this approach. Then these embryos are transferred a few months later in an endometrium that is more perfectly receptive.
For poor prognosis cases of older women with low remaining ovarian reserve, there is a huge advantage to mini-IVF over high-dose stimulation. Such patients normally yield very few eggs anyway, even with huge megadoses of gonadotropin. If they have any good-quality eggs remaining, mini-IVF is just as likely to yield as many eggs as giving huge megadoses of gonadotropin which in a sense would “poison” those eggs because of too high a level of FSH. Even in the worst case scenario, if there are no good eggs left at all, at least you can discover this with only $1,500 spent on drugs instead of $7,000 (the cost of the maximum dosage).
Clomid only prevents premature LH surges 90% of the time, so we cleverly prevent premature LH surges even in thse cases by paying close attention to each individual patient, monitoring their LH very attentively and by using both a low dose of GnRH antagonist and indocin when needed. So we never encounter the problem most physicians fear, of premature ovulation.
To get feedback from patients who have undergone treatment at our Center, click here to go to the Patient Comments page.
If you have any questions, you may call us at (314) 576-1400.
Success Stories
Facebook Live with the Ferneaus
Our Story
I wanted to first thank Dr. Silber and staff for bringing our beauitful baby girl into this world.
My husband and I tried for years to try for a baby, and we were having no hope. Until one day my sister told me about Dr. Silber, she said how good he is, and how the staff is friendly, and caring. She went to him and had great success. So I called Dr. Silber’s office, they gave me all the information I needed. Everyone was there for us, answering all our questions, and they were great at returning our phone calls right away.
We went through the mini-IVF, which was much less expensive than conventional IVF, but yet gives the very same high success, and transfered 2 embryos, and 9 months later our baby girl, Gabriella Grace, was born. 8 lbs, 9 ounches. She is a miracle of God.
Thank you again to Dr. Silber and his staff,
Michelle and Lawrence Quinones
Sioux Falls, SD

Dear Dr. Silber and Staff,
I wanted to write and thank you for making Mother’s Day 2010 one of the best days of my life. We celebrated with our amazing two-month-old twin baby girls and we wanted to extend our sincerest gratitude for helping us realize our dream to become parents.
We were both well over 40 and every doctor told us there was NO CHANCE. We soon found that local doctors were not willing to “work with us” because of my age (42 at the time we first sought help). We changed doctors 3 times and they all prescribed the same conventional treatments and tests. This went on for a whole year while I was just getting even older.

We finally figured out these doctors were trying to waste enough time to force us into using donor eggs, rather than pursue a plan that would help us try to have our OWN children. We realized that using donor eggs is a viable option for some couples but had told each doctor from the beginning that was not what we wanted. I was devastated when I realized they had basically wasted 11 precious months of our time!
Then we saw Dr. Silber. I figured if Dr. Silber was that good at thinking outside of the box, he could help a healthy 43 year old become a mother. I “googled” and found out the office was only a four and a half hour drive away.
We believe that God works through people and we had a feeling we were in the right place when we noticed a “promise” displayed on the wall that said Dr. Silber would work to the best of the ability God had given him to help people. Dr. Silber explained to us the odds of conceiving because of my age, now 43, but he also had a plan to give us a chance. Things seemed to keep telling us we were on the right track.
July 6th we found out we were pregnant. July 21st we found out it was twins! WOW!! I was treated like any other “normal” high-risk pregnancy because of my “advanced maternal age” of 43 and carrying twins. I had a very healthy pregnancy and made it to 39 weeks with what my OB described as a pregnancy better than most of her moms carrying “singletons”. We had beaten the odds.
Our very healthy and alert baby girls were born one week after my 44th birthday on March 8th! They continue to amaze us each day as we watch them grow and change. Brielle and Lillian bring such joy to our lives and we have not stopped smiling. We are so blessed.
We cannot thank you enough for your willingness to extend your expertise to successfully treat the infertility issues which older couples face.
Forever Grateful,
Dr. Dan & Lorelei Andedo
Rock Island, Illinois
Dear Dr. Silber,
My name is Ashley Snider, my husband Mike and I had tried unsuccessfully to conceive for 4 1/2 years. After 1 year of trying on our own we sought out the help of a different infertility specialist at a different facility. I underwent one surgery to address my endometriosis. We also did four IUI’s, one fresh IVF cycle, & one frozen IVF cycle, which was not useful.
It was time for a second opinion, and so we sought out Dr. Silber. Actually my husband’s cousin & his wife were going to the same doctor that we started with. They switched to Dr. Silber and highly recommended that we give him a try.
After meeting with Dr. Silber, my husband & I both really liked him. He was VERY knowledgeable and kind. You could also tell that he had the clinical background to back up the explanations that he gave us and didn’t just go by rote definitions. We knew he was going to be a great fit for us. It was like night and day with the confidence we felt between him and our first doctor.
Dr. DeRosa was the OB/GYN that worked with me from the beginning and Mindy was my nurse at Dr. Silber’s office. Dr. Silber, Dr. De Rosa, and Mindy (and all of the other staff in their office as well) were always VERY considerate, compassionate, and caring with each and EVERY encounter we had with them, whether it was meeting with them in person, talking to them on the phone, or conversing through email. They always kept us informed.
We started the process for mini-IVF in May. My frozen embryos were implanted a few months later. I just gave birth a few months ago to our beautiful baby girl Mikenley Sue. She brings us ALL the JOY in the world!!! We are FOREVER GRATEFUL to Dr. Silber and Dr. De Rosa for helping our dreams finally come true!!
Our only regret is that we didn’t find Dr. Silber sooner and before we wasted our time and money at the first facility.
Thank you Thank you Thank you to Dr. Silber, Dr. De Rosa, and the staff at both places!!!
I currently have friends and family that are also struggling to conceive and I hands down recommend Dr. Silber to all of them. I just can’t say enough nice things about him.
Thank you again from the bottom of our hearts!!
Ashley & Mike Snider (& Mikenley too)
Illinois


Dear Dr. Silber,
We tried for years to have a baby, experimenting with lots of homeopathic treatments and completing test after test in an effort to understand why we weren’t successful. We finally met with several fertility doctors, of whom Dr. Silber was the most genuine and kind. We were at our wits end and desperate for answers and hope. Mini-IVF was an unknown option until that point. Dr. Silber patiently explained our choices without any pressure, allowing us to make an informed decision that made sense for us.
What we remember most was his immediate understanding of what Nicole was going through emotionally. He also had a very different interpretation of Nicole’s blood work, noting what other doctors missed or dismissed. His theories about our infertility turned out to be entirely accurate.
The result of his empathy and expertise is our baby boy. We are happy to help him find more patients and to help patients find him. It is because of Dr. Silber that our dream of a family has been realized.
Eric & Nicole Post
St. Louis, MO

Our Story:
I owe Dr. Silber my whole world! His expertise and skill played a major part in my son Liam’s existence. As a single woman of 33 who initially visited Dr. Silber to just evaluate my fertility and who soon realized I had to act quickly to take advantage of the few remaining eggs I had left, I experienced nothing but support and encouragement from Dr. Silber and his office staff. The curse of infertility is a painful, difficult and heartbreaking situation to deal with and one that is unfortunately far too common. When time and money are of the essence and one’s impatience must be dealt with, it is comforting to know that you can trust and rely on your doctor’s years of experience and know-how to see you through. Through three mini IVF cycles, two successful retrievals, one miscarriage and one wondrous birth I can attest that miracles do happen! Miracles that get a little assistance from an amazing and genius doctor in St. Louis!
Colleen and Liam
St. Louis, MO