WHAT IS PRE-IMPLANTATION GENETIC DIAGNOSIS (PGD) OR SCREENING (PGS)?
Most of the 25,000 or so genes in the human genome have been identified and their DNA sequenced. Molecular analysis of genes is becoming simpler and more efficient. As a consequence, PGD with IVF, can now prevent couples from having to face the difficulty of giving birth to children with almost any of the genetic defects for which they might be carriers of a recessive mutation such as cystic fibrosis, muscular dystrophy, sickle cell anemia, Tay-Sachs, Gaucher’s disease, mental retardation, etc., that are a concern to every woman who ever gets pregnant. With PGD, we can also better understand the problem of recurrent, early miscarriage and the genetic errors that arise in pregnancies of older mothers.
PGD should not be construed as creating “designer babies”, an incorrect term used only by the press and not by physicians. We could not manipulate (even if we wanted to) the features or characteristics of an offspring. That is just pure fiction. All we can do is eliminate heartbreaking and devastating genetic diseases caused by mutations in either or both husband and wife. This genetic testing could be used for sex selection, but we do not believe that this is legitimate, and will not do it even though we easily could. There are two different kinds of PGD, either to eliminate parental mutations or to test for chromosomal number (aneuploidy screening). The later is used widely, but is usually more harmful than beneficial, for fascinating reasons, that I will explain later. The former, eliminating mutations of carriers of genetic disease is extremely effective and beneficial.
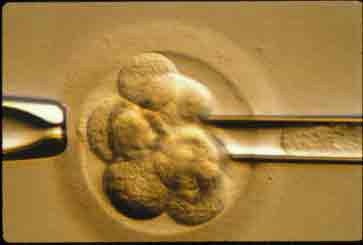
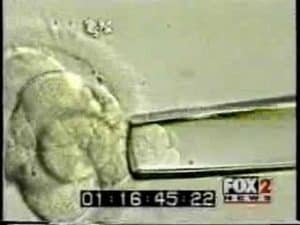
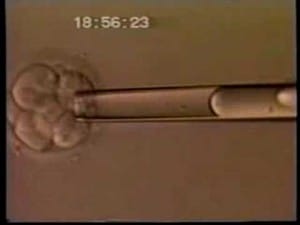
WHAT IS EMBRYO BIOPSY?
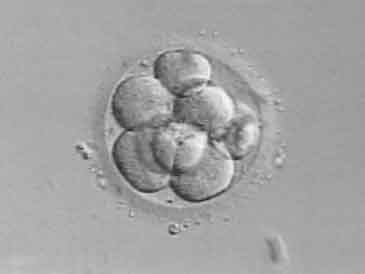
When an embryo reaches the third day of development, it normally has eight cells. One or two of these cells, called “blastomeres”, can be removed from the embryo with micromanipulation technique. The embryo is usually unharmed, and can go on to develop just as though this one cell were never removed. Of course it is not always true that there is no harm. The same can be done with the trophoblast of day 5 embryos. You can then subject those cells to genetic analysis, and know the chromosomal composition of the embryos, and if they carry a specific disease-producing mutation. Ironically it lowers the pregnancy rate. But it is a big money maker, and often is used inappropriately.
BASIC GENETIC LESSONS
DNA Testing and Single Gene Disease
This is the most appropriate indication for PGD. Everything we are physically is determined by approximately 25,000 genes located in our DNA. Your entire body so even blastocept biopsy where you can get 5 cells will vey often contain abnormal cells despite the embryo actually being normal is made up of many thousands of different proteins whose structure and orientation determine the incredible machinery of your body and brain. However, these many thousands of different proteins are in turn composed of just twenty amino acids. The variety of amino acids that theoretically could be expected to exist is unlimited. Chemists can synthesize many thousands of them. However, living nature is composed of only twenty specific amino acids, which are absolutely the same for all living things on earth. The differences between living creatures lie in the differences in the sequences of these twenty amino acids, which make up all the different proteins of which they are composed. In turn, this sequence of amino acids has been determined by the sequence of the 4 basic letters that comprise our DNA. The entire human genome represents 3 billion base pairs, or “letters”, of DNA. A specific set of combinations of three DNA letters are codes for each one of the twenty amino acids. Therefore, the order in which the DNA letters occurs on the chromosome determines the sequence of amino acids, and this, in turn, determines the proteins, which determine everything in our body. A single error in an amino acid sequence in any protein can cause a dramatic change in its structure, and a severe genetic disease like cystic fibrosis or Tay Sachs. These errors in DNA sequence can be diagnosed readily by a process (carried out in a test tube and then on an array chip, or by a process called PCR), and that is the basis of PGD for single gene genetic disease
Chromosome Testing and Aneuploidy Screening
This is a type of PGD that is frequently inappropriate, but tries to determine which embryos are more likely to get pregnant and not miscarry. I will explain it below and then why it is usually more harmful than helpful. All of our 6 billion DNA “letters” are located on forty-six chromosomes, which are coiled up inside the nucleus of every single cell in your body and are divided into twenty-three pairs, twenty-two “autosomal” pairs and one “sex” chromosome pair, the “X” and the “Y”. The child who has two X chromosomes will be a girl, and one with one Y chromosome and one X chromosome will be a boy.
For conception to occur, 23 chromosomes from the husband’s set of 46, and 23 chromosomes from the wife’s set of 46, must meet at the moment of fertilization and become an embryo with a new normal set of forty-six chromosomes. The process whereby primitive sperm cells and primitive eggs lose half of their chromosome number as they become sperm and mature eggs ready for fertilization is called “meiosis.” The aging process of eggs makes it harder for them to undergo the meiosis process than sperm. That is why the eggs from older women are less likely to result in a viable embryo, and that is also why older women are more infertile than younger women, and why older women have higher rates of miscarriage and of babies with abnormalities such as Down’s syndrome.
If there is an error in division of the egg’s chromosomes and one of the pairs of chromosomes fails to separate, then the egg will have 24 chromosomes instead of 23. In Down’s syndrome, for example, the embryo has a total of 47 chromosomes instead of 46 because it has three sets of chromosome 21 instead of the normal two sets. This kind of a chromosome error, in which one of the chromosomes has three copies instead of the proper two copies, is called “trisomy”. All of these chromosomal errors, including trisomies, monosomies, and various combinations can occur in virtually any of the chromosomes, and these errors, as a group, are called “aneuploidy.” These numerical chromosomal errors in a cell can be diagnosed by counting color signals on a slide by a process called FISH. Currently, the better techniques are array CDH or quantitative PCR.
Most of these chromosomal defects that occur in human embryos are lethal and result in either failure of the embryo to implant, or result in a miscarriage. Only rare chromosomal defects such as trisomy 21, or Down syndrome result in the actual birth of an abnormal baby, and even in trisomy 21, only 20% will result in a baby. Nothing about In-Vitro Fertilization (IVF) or ICSI, increases the risk of these chromosomal abnormalities.
Criticisms and Limitations of PGD
Single gene defects are the rare genetic diseases like cystic fibrosis or Tay Sachs (there are thousands of them), which occur in the offspring of otherwise fertile couples who are carriers, and which are diagnosed by PCR. PGD for such couples is extremely accurate today because for verification, multiple DNA sequences near the defective gene (linked markers) can be tested for, as well as the mutation itself. PGD is also very accurate for recurrent miscarriage caused by chromosomal translocations for which about 1.5% of infertile couples are carriers.
However, PGD (referred to as PGS in Europe) for routine aneuploidy screening during IVF for infertile couples has recently come under severe criticism in Europe owing to several prospective, randomized control studies in Holland and Belgium. PGS has failed to show any improvement in IVF clinical outcome per initiated cycle for advanced maternal age, nor for recurrent implantation failure. In fact it lowers the pregnancy rate and the reason for this is fascinating in terms of understanding our own peculiar human genetics.
In European studies of even younger, infertile couples, only 36% of embryos subject to PGD were found to be chromosomally normal (where two embryos are removed and tested rather than one). When embryos diagnosed as chromosomally abnormal on Day 3 (and, therefore, not transferred to the patient) were re-examined on Day 5, only 54% turned out to have that abnormality. The error rate for the FISH technique has been clearly shown to be as low as 5%. Therefore, this 50% discordance appears to be mostly due to the wide prevalence of embryo mosaicism. This means that some of the cells in many embryos are normal and some are abnormal. About 50% of human embryos in the European studies have thus been found to be mosaic. Therefore, the use of PGS may result in good embryos being discarded (diagnosed as abnormal) and abnormal embryos (diagnosed as normal) being transferred. It is fascinating that all of us, i.e. humans, “mosaics”, have a small number of chromosomally abnormal cells. Even blastocyst, where you can get 5 cells, will often contain abnormal cells, despite the embryo being actually normal.
Our experience with PGS and PGD is extensive, and we can counsel you on whether it is a good idea or not for your particular IVF cycle. In general it is best reserved for carriers of single gene disease who do not want an offspring to have such disease, and for recurrent miscarriage.
The deceptive hype about PGS or PGT-A in IVF
Although genetic testing of the embryo is very accurate for eliminating specific genetic disease you might be a carrier of, there are a lot of negatives for routine “ genetic testing “ of the embryos for chromosome counting that is often erroneously suggested to IVF patients, which will not help, and is only pushed on them so the clinic can charge more money by deceiving the patient into thinking incorrectly that this inaccurate test is accurate. You must understand that there is a difference between PGD which is very accurate, and PGS or PGT-A which can be very misleading.
We were the first to do genetic testing of embryos with our first reported case being in 1993. So we have great experience and expertise with what has become a new money spinning craze. You must understand the difference between PGS and PGD, or PGT-A and PGD. PGD means that if either the husband or the wife is a carried of a genetic mutation like cystic fibrosis or Tay Sachs or sickle cell anemia or muscular dystrophy of Huntington’s or Marfans, etc., we can do a micro biopsy of the embryo and test for such mutations, and only put back into the mother the normal embryos which do not carry this mutation. This is very accurate and relieves a great deal of justified anxiety. We have been successfully doing this since 1993.
However PGS, or what is called sometimes PGT-A, is not really genetic testing to prevent a genetic disease. It is just “chromosome counting” to try to select the embryo that is most likely to result in successful pregnancy. The problem is that it is so very inaccurate, with error rates that vary from 10 per cent to 40 per cent. The reason for this high error rate is that embryos have a variety of “normal chromosome count cells” and “abnormal chromosome count cells”. The normal cells outgrow the abnormal ones, and the area we can safely biopsy (the trophectoderm) becomes the placenta, which functions perfectly well with “abnormal” cells. So it is possible to be discarding an embryo as “abnormal” that in truth would have been a healthy baby. Furthermore it is common that an embryo diagnosed as “normal” results in no pregnancy or miscarriage. So routine genetic testing of that sort is only imposed on IVF patients to make more money. And it actually ironically lowers rather than increases the success rate per egg or embryo. In fact 4 recent studies, one by the biggest enthusiast for PGS, Dr. Munne, now admits that it does not offer any advantage for increasing pregnancy or live baby rate.
Of course we are good at these techniques and will apply them when appropriate and when the patient so requests. But we do not force it on anyone, and our results are great. IVF programs that routinely insist on doing this so called and misleading “genetic testing of embryos”, and simply deceptively only interested in making more money.
Related Information:
Preimplantation genetic screening: what is the clinical efficiency?
Improving IVF: is there a limit to our ability to manipulate human biology?
Worldwide live births following the transfer of chromosomal “Abnormal” embryos after PGT/A: results of a worldwide web-based survey
The Impact of Mosaic Embryos on Procreative Liberty and Procreative Responsibility: Time to Put Innovative Technology on “Pause”
Preimplantation genetic testing for aneuploid verses morphology as selection criteria for single frozen-thawed embryo transfer in good-prognosis patients: a multicenter randomized clinical trial
If you have any questions, you may call us at (314) 576-1400.