Genetic screening for disorder offers hope
Woman with Marfan’s didn’t want to pass it on
Front Page – St. Louis Post Dispatch, January 26, 2003
by Deborah L. Shelton
Linda Clark is 48 and seven months pregnant. With her daughter’s twins.
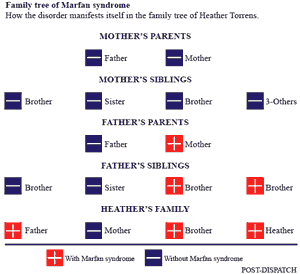
A pregnancy could have killed Clark’s daughter, Heather Torrens, because she has a severe form of a genetic disorder called Marfan syndrome. The syndrome can make pregnancy too risky.
It also can suddenly kill seemingly healthy young people. People in their prime. Star athletes.
Some 200,000 Americans have the disorder, and many don’t know it. Torrens did know, and knew that she could pass it on to her children.
So she turned to a rarely done but promising technology that could help thousands with Marfan’s.
She had embryos, created from in vitro fertilization of her eggs and her husband’s sperm, genetically screened for the disorder. Embryos free of Marfan syndrome were implanted into her mother.
“Thousands of couples are carriers of this disease,” said Dr. Sherman J. Silber, medical director of the Infertility Dr. Sherman J. Silber, medical director of the Infertility Center of St. Louis, located in Chesterfield. “Almost all of them don’t know it, and many could benefit from this technology.”
Marfan syndrome is a disorder of the connective tissue that affects the skeleton, lungs, eyes, heart and blood vessels.
It’s caused by a defective gene. People who carry the gene acquire the disease. If a parent has Marfan’s, the child has a 50 percent chance of inheriting it. In 25 percent of cases, however, the genetic mutation isn’t hereditary but occurs spontaneously at conception.
Some of the disorder’s physical characteristics are benign, such as being exceptionally tall, lean and loose-jointed. But other traits are potentially fatal, such as a defect that causes the aorta – the artery that carries blood away from the heart – to enlarge and rupture, like a balloon that stretches until it bursts. If not caught in time, the condition has a 50 percent mortality rate in the first 48 hours.
Marfan syndrome often goes undiagnosed. But if identified, it can be treated medically and corrected surgically. With intervention, people with the disorder have lived into their 70s or older.
Four years ago, when Torrens was 23, she was rushed into emergency open-heart surgery to repair her aorta after it ruptured. She almost died.
Today, she lives with an artificial heart valve and takes blood thinners.
She learned when she was 6 that the disorder ran in her family, on her father’s side. He also underwent an emergency procedure to repair his aorta and had a heart valve replaced. Torrens’ only sibling, a brother, also has Marfan syndrome. He decided on elective surgery to repair heart defects.
Heather and her husband, David Torrens, wanted to spare their children the medical complications and corrective surgeries associated with Marfan’s.
“We’re just lucky to have the technology to pre-diagnose Marfan’s so we can reduce the risk of passing it on to a baby,” David Torrens said. The couple live in Monticello, Ill., about 160 miles northeast of St. Louis.
Screening out disease
To test for Marfan syndrome, Silber, the local fertility To test for Marfan syndrome, Silber, the local fertility specialist, performed “polar body” analysis on 13 fertilized eggs. A Chicago laboratory conducted further testing. Three were free of Marfan syndrome.
Six other embryos came back with inconclusive test results requiring additional testing with a procedure called blastomere biopsy. Of the six, only three were still developing by the third day.
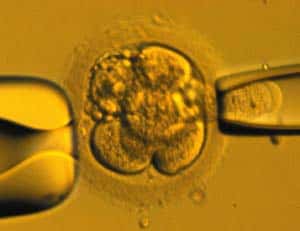
Silber removed a single cell from each of the three viable embryos. At three days old, each was about the size of a grain of sand. The cells were again sent to the Chicago laboratory, where they also were analyzed.
Removing a single cell, called a blastomere, at that stage of development doesn’t harm the embryo. A 3-day-old embryo is made up of eight genetically identical cells. If one is removed, the embryo can continue to develop normally.
Genetic screening for Marfan’s is done indirectly because no single test exists to screen for it.
Linked markers, or DNA fingerprints for Marfan’s, on chromosome 15 were identified by comparing the chromosomes of Heather Torrens, her brother and her father – all of whom have Marfan syndrome – with David Torrens, who does not.
Three unaffected embryos were implanted into Clark in the hope that at least one would develop. Two did.
Two other embryos – both with the disorder – were frozen. The rest of the 13 embryos failed to develop normally, which is not an unusual number.
Silber said the surviving embryos won’t be destroyed.
“It’s not unrealistic to think there could be treatments for such embryos based on current or future research,” he said. Silber was one of the early developers of pre-implantation Silber was one of the early developers of pre-implantation genetic diagnosis, dating back to his work with cystic fibrosis in Belgium in 1993.
Marfan syndrome is one of about 3,000 single-gene defects. Other single-gene diseases that can be screened for – and eliminated – include cystic fibrosis, muscular dystrophy, sickle cell anemia and Tay-Sachs disease.
The technology doesn’t come cheap and isn’t covered by health insurance. The Torrens paid $20,000 out-of-pocket.
Not everyone is comfortable with technology that allows genetic screening of embryos.
Medical ethicist Dr. Stephen Lefrak agrees that screening for disease falls within the ethical realm of medicine. But he fears that the technology one day could be used to create so-called designer babies.
“ At exactly what point does this particular process step over the line?” asked Lefrak, a professor of medicine at Washington University School of Medicine. “Is it OK if my wife and I use it to find only a boy to implant?”
Experts have an ethical obligation, Lefrak said, to come up with ground rules on what’s permissible and what isn’t.
Silber doesn’t use pre-implantation genetic diagnosis to screen for gender.
The idea of genetic screening for Marfan’s is widely discussed among families with the disorder.
“People are weighing advances in modern medicine that allow someone to live a longer life with Marfan’s with whether they want to use fertility technologies to avoid passing on the gene,” said Carolyn Levering, president of the National Marfan Foundation. “It’s an emotional issue.”
Some couples have decided not to have children. Others have opted for a natural pregnancy, preferring to cope with the disorder if a child inherits it. Still others, like the Torrens, select genetic screening in an attempt to avoid it altogether.
“Each case is so different,” Levering said. “Someone who comes from a family where everyone died (of Marfan’s) at 35 may feel differently than someone who comes from a family with a mild manifestation.”
A family affair
For Linda Clark, the decision has been a labor of love.
At first, she said nothing as her daughter made the rounds of obstetricians and fertility specialists to determine her options for having a family. Clark didn’t want to interfere, but she also knew a pregnancy would put her daughter’s life in peril. If her daughter chose to go with a surrogate mother, she wanted to be that person.
Without telling her daughter, Clark asked her own doctor during an annual exam, if she was healthy enough to serve as a surrogate mother and carry a baby to term. He said yes.
Afterward, Clark sat down with her daughter.
“After we discussed all the options, I said, ‘Here’s one possibility,’ and put it on the table,” Clark recalled.
The offer came as a surprise to her daughter.
“I just about fell out of my chair,” said Torrens, a part-time bank teller. “I thought it was amazing that she was willing to do something like that.”
“It’s not that I have to have grandkids,” said Clark, of Decatur, Ill. “But I’m also getting a gift by helping to enlarge our family.”
Despite all her mother’s help, the pregnancy has not been problem-free for Torrens.
She was hospitalized in July for two weeks – five days in intensive care – after a procedure to remove eggs from her ovaries caused her to bleed heavily into her abdomen. The problem was a complication of Marfan syndrome.
Today, Torrens lives the unique life of a prospective mother who is expecting twins but is not pregnant.
“The babies are kicking and flopping around,” she said. In front of her, spread across the kitchen table, atop the couple’s wedding pictures, were photos of the babies taken when they were just embryos.
“I’d like to feel the babies kicking me in the rib,” she said, and then laughed. “But a lot of people say, ‘No, you’re doing it the right way!’”
Clark is expected to give birth in mid-March.
As that special day approaches, Clark expresses surprise that people view the pregnancy as anything unusual.
“If you have a chance to give a child the best life you can,” she said, “most people – if they really think about it – would choose to do that.”
Front Page – St. Louis Post Dispatch
January 26, 2003
Heather’s mother delivered Heather’s healthy twins (boy and girl) on February 13, 2003. Both children are normal without any genetic trace of Marfan’s disease.




