CF Life
by Janis Kelly, editor of CF Life
Men with cystic fibrosis (CF) are known to be sterile, but a new procedure now allows most to become fathers, according to Sherman J. Silber, MD, Director of the Infertility Center of St. Louis (Missouri). Most men with CF produce perfectly good sperm. The problem is that the duct that should carry sperm from the testis is not complete. Dr. Silber’s approach rescues healthy sperm from the bit of duct left near the testis and uses those sperm for in vitro (“in the test tube”) fertilization of eggs removed from the prospective mother. The resulting embryos are then transferred into the woman 5 uterus to develop as usual.
“All men with CF have congenital absence of the vas deferens (CAVD),” Dr. Silber explained. “Men with CF are not sterile because they don’t produce sperm, or because their sperm ducts are plugged up with secretions, as one might imagine. They are sterile because their sperm ducts do not develop at all.”
In 1986 Dr. Silber and colleagues began working on a way to get around this problem. The result combines three procedures. The first is MESA (micro- surgical epididymal sperm aspiration), the second is ICSI (intracytoplasmic sperm injection), and the third is transfer of the fertilized egg into the womb.
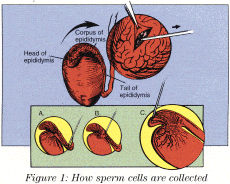
MESA is used to retrieve sperm (Figure 1). A small incision is made in the scrotum, and the epididymis (sperm duct) is exposed. A tiny incision is made with microscissors in the part of the duct near the testis. A micropipette is then used to aspirate sperm cells from the duct. This procedure takes about 20 minutes and is done under local anesthesia.
These sperm usually would not be able to fertilize an egg, because they have missed their trip down the sperm duct and so are not completely mature. The solution to this problem is ICSI. “We pick up a single sperm at a time and inject one sperm into each egg. This makes up for the fact that these sperm do not have the strength to fertilize the eggs themselves. Once they are put into the egg, they work fine,” Dr. Silber said.
Before the sperm are taken, the woman is given 10 to 14 days of hormone injections, which cause the ovaries to prepare several eggs at a time for fertilization. Dr. Silber puts a needle in through the vagina and aspirates the fluid and egg from each of the “ready” follicles in the ovary.
“Next we pick the sperm up one at a time from a little droplet under a microscope, using very tiny instruments and pipettes. We move a single sperm to a little droplet that holds one egg and inject it into that egg’s cytoplasm. A micropipette holds the egg in place during this injection.”
“Once all the eggs are fertilized,” Dr. Silber continued, “they are put into an incubator for two days. Then they are checked to see that they are developing properly We then pick three or four of the best embryos to transfer into the woman’s womb.
The chance of any single fertilized egg becoming a baby is about 15%. This is a basic fact of human biology. Even couples without CF who are having unprotected sex have only about a 15% chance of pregnancy each month,” Dr. Silber explained. That is why more than one embryo is usually transferred at a time, to increase the pregnancy rate per treatment cycle.
Dr. Silber has used the ICSI method in about 400 women, including about 150 who have CF “The pregnancy rate depends on the woman’s age,” he said. “If the woman is under 30, the pregnancy rate is over 50% per treatment. If the woman is between 30 and 36, the pregnancy rate goes down to about 35% (Table 1). Most couples should have a successful pregnancy within three tries if the woman is 30 years old or younger.” He generally does not recommend in vitro fertilization for women over the age of 40, because of the low success rate.
“No matter how advanced the CF is, we can always get live sperm from a man. Whether he wants to conceive a child is thus more a matter of social and psychological concerns. Is he going to be around to raise the child?”
This method costs about $10,000 per treatment cycle at Dr. Silber’s clinic. Insurance coverage is a patchwork and largely depends on whether your state insurance commission requires companies to cover infertility treatment.