“REPRODUCTIVE BIOLOGY”
THE SCIENTIST; Volume 10, No. 22 November 11, 1996
S.J. Silber, Z.P. Nagy, J. Liu, H. Godoy, R Devroey, A.C. Van Steirteghem, “Conventional in vitro fertilization versus intracytoplasmic sperm injection for patients requiring microsurgical sperm injection,” Human Reproduction, 9:1705-9,1994. (Cited in more than 50 papers as of October 1996)
Comments by Sherman J. Silber, St. Luke’s Hospital, St. Louis

Infertility Center of St. Louis
at St. Luke’s Hospital
For years, one of the most frustrating causes of male infertility was the congenital absence of the vas deferens, in addition to other irreparable obstructions. Affected men usually can make sperm, but the sperm have no way of leaving the epididymis and reaching the egg. Doctors can remove sperm from the epididymis-a long, coiled microscopic tube that carries sperm from the testicle to the vas deferens-for in vitro fertilization. However, success rates in the past for the procedure have been poor.
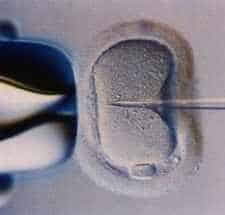
In 1992, Sherman Silber, director of in vitro fertilization and microsurgery at the Infertility Center of St. Louis at St. Luke’s Hospital, along with colleagues there and at Brussels Dutch Speaking Free University, developed a technique aimed at circumventing such problems. The technique, intracytoplasmic sperm injection (ICSI), entails injecting a single sperm into an egg.
According to Silber, when sperm are removed from the epididymis, such “retrieved sperm” have a low fertilization and pregnancy success rate when used in conventional in vitro fertilization (IVF), which typically entails mixing sperm and egg in a laboratory dish.
This paper is the first report in which the researchers used ICSI with sperm retrieved from the epididymis of males with otherwise irreparable obstructive azoospermia. The sperm achieved a normal fertilization and pregnancy success rate.
In 1988, Silber and his colleagues began surgically retrieving sperm from the blocked epididymis to use in IVF. But the results were poor; only 7 percent of the fertilizations progressed to pregnancy.
Silber cites several causes of male sterility. Some 40,000 men in the United States have congenital absence of the vas deferens. Another 40,000 have inflammation of the epididymis. “We estimate [there are] about 200,000 who suffer from obstructive azoospermia causing sterility.”
Silber believes the paper has been cited so frequently because the work represents a “gigantic breakthrough for male infertility.”
In another paper (S.J. Silber et al., Human Reproduction, 10:148-52, 1995), he was able to show that using ICSI with sperm from a small piece of removed testicular tissue, he could still obtain fertilization and pregnancy rates that were fairly normal. Such sperm are normally even less motile and weaker than epididymal sperm.
Subsequently, the researchers found that even men with nonobstructive azoospermia, in which they are not making sperm, still produced immature sperm, or spermatids (S.J. Silber et al., Fertility and Sterility, 66:110-17, 1996). “Now we can deal not only with a low sperm count, but even [with] a zero sperm count, and the man can be fertile,” he says, referring to patients who do not produce mature sperm. “You inject those immature sperm into the [female partner’s] egg and the fertilization and pregnancy rates are no different than normal,” Silber says. “Those three papers span a progression: retrieving epididymal sperm from those with obstructon to retrieving testicular sperm from those who don’t have the ductwork to retrieving it from those who can’t make the sperm.
Silber believes the revolution in genetic testing will play a huge role in the future of fertility research. “Preimplantation genetic diagnosis is the next step in development,” he notes.
According to Silber, if the human genome is sequenced by 2004, there will be better techniques to test the human blastomere for genetic disease. What’s more, “in five to 10 years micromanipulation surgical technique-really microsurgery on the embryo-will result in embryo biopsy.” This, Silber says, will help couples who are at risk of passing genetic disease to their offspring.
See also:


