Sherman J. Silber, MD; Mark P. Connolly, MHE; Michael S. Pollard, PhD; Stijn Hoorens, MSc; Brian R. Kaplan, MD; and Selwyn P. Oskowitz, MD
A Lifetime Tax Calculation – The American Journal of Managed Care
September 2008
Objective: To evaluate whether lifetime future net tax revenues from an in vitro fertilization (IVF)-conceived child are substantial enough to warrant public subsidy relative to the mean IVF treatment costs required to obtain 1 live birth.
Study Design: Mathematical generational accounting model.
Methods: The model estimates direct financial interactions between the IVF-conceived child and the government during the child’s projected lifetime. In the model, we accrue IVF costs required to conceive the child to the government, and then we estimate future net tax revenue to the federal and state governments from this individual, offset by direct financial transfers from the government (eg, child allowances, education, Medicare, and Social Security). We discount lifetime costs and gross tax payments at Treasury Department rates to establish the present value of investing in IVF. We applied US Congressional Budget Office projected changes in tax rates over the course of the model.
Results: An IVF-conceived child, average in every respect (eg, future earnings, healthcare consumption, and life expectancy), represents a net positive return to the government. Based on an average employed individual born in 2005, the projected net lifetime tax contribution is US $606,200. Taking into consideration IVF costs and all direct financial interactions, the net present value is US $155,870.
Conclusions: Lifetime net taxes paid from a child relative to the child’s initial IVF investment represent a 700% net return to the government in discounted US dollars from fully employed individuals. This suggests that removing barriers to IVF would have positive tax benefits for the government, notwithstanding its beneficial effect on overall economic growth.
(Am J Manag Care. 2008;14(9):598-604)
The past decade has witnessed a dramatic increase in the demand for assisted reproductive technology (ART ) such as in vitro fertilization (IVF).1,2 Increasing demand for ART is related to increased infertility in modern populations, which may be attributed to couples’ delaying efforts to get pregnant until they are older and less fertile, increasing obesity in the United States, sexually transmitted diseases, low sperm count, and the stress of modern daily life.3-6 In countries where generous funding for fertility treatments is available, ART accounts for 4% to 6% of national births every year.1,2 When the proportion of children born every year from ART is couched within the population aging debate faced by many countries and the economic consequences this creates, policy analysts have started to investigate the role that fertility treatments could play in solving severe demographic issues associated with an aging population and the resulting insolvency of Social Security.7-10
Despite increasing demand for ART treatments, financial constraints are causing many national health providers and private insurers to limit access, and most couples must pay out-of-pocket for these services.11 For couples unable to afford ART , the options are limited; consequently, many withdraw from treatment or choose not to pursue treatment because of costs.12-14 Furthermore, the established relationship between affordability and utilization of services would suggest that many couples are unable to receive treatment, with the likely consequence of fewer children being born every year.15
The economic and health consequences of financial barriers to medical treatment are frequent topics of interest for health economists and policy analysts.16-18 With respect to ART services, treatment barriers create an additional issue, as successful use of this technology leads to the creation of human life that would not have been born were the technology not available. The immediate benefit of ART success is to fulfill a couple’s desired family size, which leads to quality-of-life improvements. However, what is less well characterized is the economic effect that IVF-conceived children will make once they become economically active adults.
Methods
To assess the economic consequences of IVF-conceived children, we developed a mathematical model that explores the lifetime financial transactions between a single individual conceived by IVF and the government under a theoretical assumption that the government paid standard fees for that IVF treatment. To evaluate whether investing in IVF represents sound fiscal policy for the government, we theoretically assigned IVF costs to the US government in the model. The methods applied herein are based on generational accounting (GA) methods developed by Kotlikoff et al19,20 and Sturrock21 and used by treasury departments, including the US Congressional Budget Office, to assess whether current fiscal policies will adversely affect future generations (ie, shift costs to future generations). In this article, we describe a GA model to assess future net tax revenues derived from a hypothetical IVF-conceived child to establish whether policies that increase access to IVF treatment would generate long-term economic benefits. It is envisaged that this analysis can inform government and nongovernment agencies with a vested interest in future population age structures. Such an analysis is urgently needed in view of declining birthrates, increasing numbers of aging retired persons, and the predicted insolvency of Social Security.
Based on the US GA model developed by Kotlikoff,19 a basic mathematical model was developed taking the perspective of the US government to estimate the discounted lifetime net tax contribution derived from a single individual. The model describes the financial position between the child and the government during the child’s projected lifetime. For comparison, the model estimates lifetime net tax contributions for a naturally conceived versus an IVF-conceived child, where the major cost difference is assumed to be IVF treatment costs and any extra costs related to the child’s care. In this model, we assign IVF costs to the government to assess the merits of funding such a policy. All direct government expenditures and tax contributions were discounted using Treasury Department rates. Conceptually, there are 3 broad stages in lifetime financial interactions, each with differing components of the financial exchange, as follows: (1) early life, when the government primarily contributes resources to individuals through child tax credits, healthcare, and educational expenses; (2) employment, when individuals begin returning resources to the government through federal, state, and local taxes; and (3) retirement, when the government expends additional resources on Social Security and old-age programs. Two general models are estimated. The first model assumes that individuals graduate from high school and then follow the average higher education, employment, and unemployment trends (hereafter referred to as average employment). The second model assumes full-time education from ages 6 to 19 years, with full-time employment from age 20 years until retirement at age 65 years (hereafter referred to as full employment). The models assume that successful IVF treatment results in a single live birth (with a mean life expectancy of 79 years) and that the child is identical to a naturally conceived individual.22,23 In all scenarios, the model includes hospital delivery costs, taking into consideration additional costs frequently accrued to IVF-conceived children attributed to low birth weight.24,25 Age-graded government expenses and tax contributions were assessed across a hypothetical individual’s lifetime to derive discounted lifetime net tax contributions using net present value (NPV) calculations and undiscounted lifetime net tax contributions. Following similar GA calculations used to assess US immigration policy, we consider various costs generated and taxes paid.26,27
Expenditures
Two broad categories of federal and state government expenditures are considered, congestible goods and transfer programs.28 Congestible goods have nonzero marginal costs and include expenditures such as roads, fire and police protection, airports, and sewers. Transfer programs include all government expenditures that can be assigned to specific individuals such as Social Security, Supplemental Security Income, Medicare, Medicaid, Aid to Families With Dependent Children, public assistance, food stamps, unemployment benefits, disability benefits, subsidized school lunch programs, and public education at all levels. There is also a child tax credit associated with individuals until age 17 years.
Revenues
Revenues collected by the government include federal and state income tax (the national mean rate in this model), corporate tax, excise tax, Federal Insurance Contributions Act tax, Supplemental Medical Insurance contributions, federal retirement tax, property tax, and sales tax. To calculate the accounting models, age profiles of each expenditure and revenue component were identified from existing data sources. Because the models describe financial interactions across an individual’s lifetime, these age profiles are adjusted to account for depreciation of money over time through the application of a discount rate. The US Congressional Budget Office 2007 projections were used as the basis for estimates of inflation, individual earnings increases, tax rate increases, increases in Supplemental Medical Insurance revenue, and Medicare and Medicaid expenditures.29 Increases in expenditures on schooling are based on historical rates of increase.30 Beyond the period for which these long-term forecasts are available, we assume that particular components grow to keep pace with demographic and productivity growth. A discount rate of 4% was applied to lifetime tax revenue and transfer payments. The discount rate was compounded continuously.
IVF Treatment Costs. The mean IVF treatment costs to produce a live birth are considered herein as a further expense unique to an individual conceived using IVF. The national mean cost per IVF treatment cycle in 2003 is US $12,400.31 Cost per live birth is calculated as the mean cost per cycle divided by the age-adjusted probability of a live birth, where the treatment efficacy is known to vary primarily by the age of the mother (ie, lower success rates with older age) and by other factors.31-34 The age-adjusted cost per live birth is given in Table 1.

Data Sources. Analyses are based primarily on 2 waves of the annual March Current Population Survey.35 The Current Population Survey is a monthly survey of about 50,000 households conducted by the Bureau of the Census for the Bureau of Labor Statistics and is the primary source of information on the labor force characteristics of the US population. The sample is representative of the civilian noninstitutional population. Estimated sales tax revenue is obtained from the Consumer Expenditure Survey, also conducted by the Bureau of Labor Statistics. Government expenditures on congestible goods are obtained from the US Statistical Abstract, following prior work.26 Educational expenditures are taken from the Digest of Education Statistics.30
Calculation of NPV. Given the baseline assumptions for the age profiles of expenditures and revenues, the net financial exchange of an individual at any age is derived in the accounting models simply as the discounted sum of all the economic components up to that age. Specifically, lifetime individual NPV is the discounted sum of all revenues to the government at all ages minus expenditures at all ages as follows:
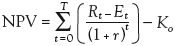
where Rt indicates the sum of all revenues accruing from the individual at age t; Et, the sum of all expenditures on the individual at age t; r, the rate of discount; T, the life expectancy at birth; and Ko, the initial direct costs of IVF in the base period. For individuals conceived by IVF, the direct cost of achieving a live birth is included in the expenditures as consisting of the cost of IVF treatment and the mean additional hospital costs associated with low birth weight attributed to IVF infants.24,25
Results
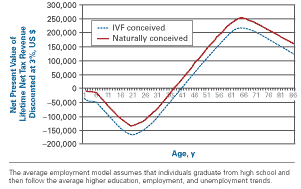
The projected lifetime net tax contribution trajectories for an average employment naturally conceived child and for an IVF-conceived child are shown in the Figure. There is a net increase in government revenue by age 37 years for naturally conceived children versus by age 40 years for an IVF-conceived child. The additional costs attributed to conceiving an IVF child are shown as an increased cost at birth. In all simulations, the financial position between the child and the government changes as the child enters the workforce and again at the point of leaving full-time employment, with a net profit to the taxing authority. In vitro fertilization coverage represents a minor component of the net cost for creation of new taxpayers.
The projected combined returns to the federal and state governments in lifetime net tax contributions from an IVFconceived child and from a naturally conceived child are given in Table 1. For a naturally conceived child, the mean discounted lifetime tax contribution amounts to US $292,285 for full employment; the projected net undiscounted lifetime tax contribution for a full employment individual born in 2005 is US $1,103,000 (Table 2). For IVF-conceived children, the net undiscounted lifetime tax contribution is similar to that for naturally conceived children even after IVF investment costs are factored into the analysis.
The age at which the financial position between a naturally conceived child and an IVF-conceived child changes with respect to the taxing authority is given in Table 1. We have labeled this as the breakeven age to highlight the age at which the government has recouped all direct financial transfers (discounted) in the early years to achieve working-age participation. Assuming full employment, the breakeven ages with net profit to the government are 34 years for naturally conceived children and 36 to 38 years for IVF children conceived to mothers younger than 41 years. The difference in the breakeven age for IVF-conceived children compared with naturally conceived children differs by 2 to 5 years depending on variations in increasing IVF investment costs attributed to older mothers.12,32
Discussion
The approach used in this model assesses medical costs attributed to conceiving an IVF child as an investment required to achieve a live birth with consequent long-term economic returns. It is likely that the conceptual model described herein is of most relevance to countries with nationally funded health services where the taxing authority and the health service are 2 components of the overall government. Under these circumstances, the national health service pays for or provides IVF treatment, and the tax authority will collect tax revenue from the IVF-conceived child when he or she reaches working age.
There are obvious flaws in applying this methodological approach in the United States, where there is a clear separation between the payer (eg, infertile couples and private insurers) and the beneficiary of future tax payments from IVF children (ie, Internal Revenue Service). Despite these shortcomings, we have positioned IVF medical costs as accruing to the government to inform government health policy in this area and to stimulate debate.

The analysis described herein has taken the perspective of the taxing authority, where net tax contributions (ie, gross tax contributions minus direct government transfers and congestibles) are the sole economic variable considered. Because our approach has taken the perspective of the government, there are limitations to our model, which does not consider the broader economic benefits that individuals contribute to a country’s economic growth. Consequently, the analysis presented herein is an underestimate of the true economic contributions that an individual has on the economy as a whole because we have not considered the gross domestic product contribution brought about by the increased demand for goods and services generated by this individual.
The methods applied in our work are based on GA, a method frequently used by government treasury departments as an alternative to the more commonly applied deficit accounting, which only considers current year accounts. Using GA helps bridge the gap between what has been promised in the future (eg, Medicare and Social Security payments) in relation to future revenue generated predominantly through taxation. From the government revenue–generating perspective, the number of taxpayers and the mean tax contribution per individual are relevant, as well as the importance of current birthrates, which will directly influence the number of taxpayers in the future and, depending on future spending promises, the tax rates paid by future generations.19,20 Considering the effect that birthrates have on future fiscal imbalances between current and future generations, we believe that our approach is acceptable for evaluating IVF technology because of its established ability to significantly affect national birthrates.1,2,9
Several simplifying assumptions were made during the course of the work that can be challenged. In particular, clinnicians may criticize the assumption that IVF children are identical to naturally conceived children. Although we have adjusted initial costs to compensate for lower birth weight, we do not treat the subsequent education and employment trajectories of these individuals differently from those of naturally conceived individuals. Furthermore, additional medical costs frequently arise as a result of multiple pregnancies and premature birth. However, it is likely that much of this increased risk can be mitigated by a reduction in embryos transferred and multiple births when the burden of success is shared by a third-party payer.36,37 For example, following the Belgian example, the government agreed to fund up to 6 IVF cycles for every infertile couple, while simultaneously regulating the number of embryos transferred in each cycle.38 Support of IVF allows the funding authority to limit the number of embryos transferred and to obviate any of the extra risks associated with patient-funded IVF. The net result of this policy change for Belgium was a cost saving attributed to a reduction in multiple pregnancies.
In our model, we assumed that a child born from IVF would achieve average lifetime income earnings, which may be an oversimplification of future earnings based on current IVF utilization. What is known at present is that those seeking treatment for infertility and undergoing IVF are not representative of the US population because racial/ethnic and economic factors define treatment-seeking behavior.39,40 In the current environment, which is dependent on out-of-pocket payments, those accessing and using IVF services are overrepresented by individuals with higher socioeconomic backgrounds and with the financial means to pay for IVF.41,42 As a consequence of an increased proportion of higher socioeconomic families accessing infertility treatments, IVF children are more likely to achieve higher socioeconomic status in their lifetimes.43 This is further supported by research suggesting that IVFconceived children obtain higher academic scores compared with naturally conceived children.44 This would suggest that in the present IVF access environment children conceived through IVF are likely to make future tax contributions above the mean figures described in our results.
The disparity in IVF utilization based on socioeconomic status raises questions regarding what could happen if barriers to IVF were lowered, allowing for a broader range of socioeconomic groups to access treatment. In our model, the calculations are based on the statistical mean for lifetime income, which is based on income from all socioeconomic groups, low and high. On this basis, if an increased proportion of families of lower socioeconomic status accessed IVF, this would not affect the conclusions of our work because the lower earning capacity has already been accounted for in the average lifetime financial calculations.
One of the underlying aims of this research is to highlight that economic barriers limit access to infertility treatments and that costs attributed to infertility are dependent on the perspective and the period during which costs and benefits are observed. Based on our analysis, we suggest that discounted future net tax contributions derived from IVFconceived children could be used to justify government funded IVF programs. Our work also highlights that there is a cost associated with not treating infertility in the form of lost tax revenue, which to the best of our knowledge has never been quantified. This study is not the first application of GA principles to address important policy questions. Previous explorations using GA models have evaluated the effect of US immigration policies on government fiscal imbalances.45 Although it is tempting to compare our findings with those from immigration policy, we believe that this is not feasible because immigration and fertility policies are shaped by different social and political issues, of which economics is only one of many components.
Based on projected tax revenue to the government, our analysis suggests that removal of financial barriers to IVF treatment, which may lead to increases in birthrates, could help to achieve broader demographic and economic policy goals. We acknowledge that this proposition may be provocative, but it is not without precedent. Within the United States, under the current system of sporadic IVF insurance coverage and various state mandates, a demographic effect has already been observed. In a recent study by Schmidt,46 it was shown that in those states with legislated mandates there is an increased birthrate for women older than 35 years compared with states without mandates. Going a step further, in countries such as South Korea and Israel facing demographic crisis and regional instability, respectively, IVF funding policy is viewed as a pronatalist tool for influencing population growth.47,48
Conclusions
The principal aim of this research was to assess the net tax contributions of an IVF-conceived child, with the intention of informing future policy directives that may influence access to fertility treatments. In reality, there are many good reasons to justify improved IVF access, including medical need, equity, and respect for an individual’s human right to a family, and reproductive rights. However, in many countries, including the United States, access to fertility care is limited, and many couples are unable to afford treatment. Based on the results shown herein, one could easily argue on the basis of economics that financial or legislative barriers to IVF treatments for infertile couples should be removed.
Take-away Points
- Financial and legislative barriers to fertility treatments prevent many couples from achieving their desired family size, resulting in fewer children being born.
- Taking the perspective of the government, fewer children born in current generations represents a loss in future tax revenue that would arise from these children after they enter the workforce.
- The costs attributed to in vitro fertilization (IVF) treatment are insignificant in light of the lifetime net tax contributions of IVF-conceived children.
- Minimizing barriers to fertility treatments is likely to have long-term economic benefits that need to be considered when making IVF funding decisions.
Acknowledgments
We are grateful for comments and guidance provided by Dr Craig Currie from Cardiff Medical School.
Author Affiliations: From Ferring International Center (MPC), St Prex, Switzerland; the RAND Corporation (MSP), Santa Monica, CA; the RAND Corporation (SH), Cambridge, England; the Fertility Centers of Illinois (BR K), Chicago; the Boston IVF and the Department of Obstetrics, Gynecology and Reproductive Biology, Harvard Medical School (SP O), Boston, MA; and the Infertility Center of St Louis at St Luke’s Hospital (SJS), St Louis, MO.
Funding Source: This study was funded by the not-for-profit RAND Corporation and by Ferring International Center.
Author Disclosure: Mr Connolly is an employee of Ferring International Center, a funder of this study. Dr Pollard and Mr Hoorens report receiving grant funding from Ferring International Center. Dr Oskowitz is a board member of Columbia Labs, a manufacturer of hormones used in IVF treatment, and reports owning stock in that company. Drs Kaplan and Silber report no relationship or financial interest with any entity that would pose a conflict of interest with the subject matter of this article.
Authorship Information: Concept and design (MPC, MSP, SH, SJS); acquisition of data (MSP); analysis and interpretation of data (MPC, MSP, SPO, SJS); drafting of the manuscript (MPC, MSP, SH, BRK, SPO, SJS); critical revision of the manuscript for important intellectual content (MPC, MSP, SH, BRK, SPO, SJS); statistical analysis (MSP); obtaining funding (MPC, MSP, SH); administrative, technical, or logistic support (MPC); and supervision (MPC).
Address correspondence to: Sherman J. Silber, MD, Infertility Center of St Louis at St Luke’s Hospital, 224 S Woods Mill Rd, St Louis, MO 63017.
References
- Andersen AN, Gianaroli L, Felberbaum R, de Mouzon J, Nygren KG; European IVF-Monitoring Programme (EIM) for the European Society of Human Reproduction and Embryology (ESHRE). Assisted reproductive technology in Europe, 2002: results generated from European registers by ESHRE. Hum Reprod. 2006;21(7):1680-1697.
- Andersen AN, Goossens V, Gianaroli L, Felberbaum R, de Mouzon J, Nygren KG. Assisted reproductive technology in Europe, 2003: results generated from European registers by ESHRE. Hum Reprod. 2007;22(6):1513-1525.
- Heck KE, Schoendorf KC, Ventura SJ, Kiely JL. Delayed childbearing by education level in the United States, 1969-1994. Matern Child Health J. 1997;1(2):81-88.
- National Institute for Health and Clinical Excellence. Clinical Guideline 11. Fertility: assessment and treatment for people with fertility problems. February 2004. http://www.nice.org.uk/Guidance/CG77/Guidance/pdf/English. Accessed November 17, 2007.
- Gunnell DJ, Ewings P. Infertility prevalence, needs assessment and purchasing. J Public Health Med. 1994;16(1):29-35.
- Vayena E, Rowe PJ, Griffin PD, eds. Current practices and controversies in assisted reproduction: report of a meeting on “Medical, Ethical and Social Aspects of Assisted Reproduction” held at WHO headquarters in Geneva, Switzerland, 17-21 September 2001. http://www.who.int/reproductive-health/infertility/report.pdf. Accessed November 4, 2007.
- Grant J. Hoorens S. The new pronatalism? Public Policy Res. 2006;13(1):13-25.
- Bloom DE, Canning D, Sevilla J. The Demographic Dividend: A New Perspective on the Economic Consequences of Population Change. Santa Monica, CA: RAND Corp; 2003.
- Hoorens S, Gallo F, Cave JA, Grant JC. Can assisted reproductive technologies help to offset population ageing? An assessment of the demographic and economic impact of ART in Denmark and UK. Hum Reprod. 2007;22(9):2471-2475.
- Sunde A. Europe’s declining population and the contribution of ART. Pharm Policy Law. 2007;9(1-2):79-89.
- Jones HW, Cohen J. Insurance coverage (chapter 2). Fertil Steril. 2004;81(suppl 4):17-18.
- Collins J. An international survey of the health economics of IVF and ICSI. Hum Reprod Update. 2002;8(3):265-277.
- Rajkhowa M, McConnell A, Thomas GE. Reasons for discontinuation of IVF treatment: a questionnaire study. Hum Reprod. 2005;21(2):358-363.
- Farley Ordovensky Staniec J, Webb NJ. Utilization of infertility services: how much does money matter? Health Serv Res. 2007;42(3,pt 1):971-989.
- Collins J. Cost-effectiveness of in vitro fertilization. Semin Reprod Med. 2001;19(3):279-289.
- Finkelstein BS, Silvers JB, Marrero U, Neuhauser D, Cuttler L. Insurance coverage, physician recommendations, and access to emerging treatments: growth hormone therapy for childhood short stature. JAMA. 1998;279(9):663-668.
- Hadley J, Steinberg EP, Feder J. Comparison of uninsured and privately insured hospital patients: condition on admission, resource use, and outcome. JAMA. 1991;265(3):374-379.
- Soumerai SB, McLaughlin TJ, Ross-Degnan D, Casteris CS, Bollini P. Effects of limiting Medicaid drug-reimbursement benefits on the use of psychotropic agents and acute mental health services by patients with schizophrenia. N Engl J Med. 1994;331(10):650-655.
- Kotlikoff LJ. Generational Accounting. New York, NY: Free Press; 1992.
- Cardarelli R, Sefton J, Kotlikoff LJ. Generational accounting in the UK. Economic J. 2000;110(467):F547-F574.
- Sturrock J. Who Pays and When? An Assessment of Generational Accounting. Washington, DC: Macroeconomic Analysis Division, Congressional Budget Office, Congress of the United States; 1995.
- Bonduelle M, Liebaers I, Deketelaere V, et al. Neonatal data on a cohort of 2889 infants born after ICSI (1991-1999) and of 2995 infants born after IVF (1983-1999). Hum Reprod. 2002;17(3):671-694.
- Silber SJ. Will my baby be normal? In: How to Get Pregnant. New York, NY: Little Brown & Co; 2005:273-324.
- Almond D, Chay KY, Lee DS. The costs of low birth weight. Q J Econ. 2005;120(3):1031-1083.
- Schieve LA, Ferre C, Peterson HB, Macaluso M, Reynolds MA, Wright VC. Perinatal outcome among singleton infants conceived through assisted reproductive technology in the United States. Obstet Gynecol. 2004;103(6):1144-1153.
- Lee RD, Miller TW. The current fiscal impact of immigrants and their descendants: beyond the immigrant household. In: Smith JP, Edmonston B, eds. The Immigration Debate: Studies on the Economic, Demographic, and Fiscal Effects of Immigration. Washington, DC: National Academy Press; 1998:183-205.
- Smith JP, Edmonston B, eds; National Research Council. The New Americans: Economic, Demographic and Fiscal Impacts of Immigration. Washington, DC: National Academy Press; 1997.
- MaCurdy T, Nechyba T, Bhattacharya J. An economic framework for assessing the fiscal impacts of immigration. In: Smith JP, Edmonston B, eds. The Immigration Debate: Studies on the Economic, Demographic, and Fiscal Effects of Immigration. Washington, DC: National Academy Press; 1998:13-65.
- Congressional Budget Office. The budget and economic outlook: fiscal years 2008-2017. http://www.cbo.gov/ftpdocs/77xx/doc7731/01-24-BudgetOutlook.pdf. Accessed November 2, 2007.
- Snyder TD, Tan AG, Hoffman CM. Digest of Education Statistics 2005 (NCES 2006-030). Washington, DC: National Center for Education Statistics, US Dept Education; 2006.
- Wright VC, Schieve LA, Reynolds MA, Jeng G; Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, Centers for Disease Control and Prevention (CDC). Assisted reproductive technology surveillance: United States, 2002. MMWR Surveill Summ. 2005;54(2):1-24.
- Centers for Disease Control and Prevention. Assisted Reproductive Technology Success Rates: National Summary and Fertility Clinic Report (2004). Atlanta, GA: Centers for Disease Control and Prevention, US Dept Health and Human Services; 2006.
- Lintsen AME, Eijkemans MJC, Hunault CC, et al. Predicting ongoing pregnancy chances after IVF and ICSI: a national prospective study. Hum Reprod. 2007;22(9):2455-2462.
- Callahan TL, Hall JE, Ettner SL, Christiansen CL, Greene ME, Crowley WF. The economic impact of multiple-gestation pregnancies and the contribution of assisted-reproduction techniques to their incidence. N Engl J Med. 1994;331(4):244-249.
- Current Population Survey. US Department of Labor, Bureau of Labor Statistics, panel data 2003 and 2004. http://www.bls.gov/cps/publications.htm. Accessed November 2, 2007.
- Smith S, Pfeifer SM, Collins JA. Diagnosis and management of female infertility. JAMA. 2003;290(13):1767-1770.
- Frankfurter D. To insure or not to insure: that is the question. Fertil Steril. 2003;80(1):24-26.
- Ombelet W. Access to assisted reproduction services and infertility treatment in Belgium in the context of the European countries. Pharm Policy Law. 2007;9:189-201.
- Chandra A, Stephen EH. Impaired fecundity in the United States: 1982-1995. Fam Plann Perspect. 1998;30(1):34-42.
- White L, McQuillan J, Greil AL. Explaining disparities in treatment seeking: the case of infertility. Fertil Steril. 2006;85(4):853-857.
- Bitler M, Schmidt L. Health disparities and infertility: impacts of state-level insurance mandates. Fertil Steril. 2006;85(4):858-865.
- Stephen EH, Chandra A. Use of infertility services in the United States: 1995. Fam Plann Perspect. 2000;32(3):132-137.
- Ashenfelter P, Layard R, eds. Handbook of Labor Economics. Vol 1-3. Oxford, England: Elsevier North Holland; 1986.
- Leunens L, Celestin-Westreich S, Bonduelle M, Liebaers I, Ponjaert-Kristoffersen I. Cognitive and motor development of 8-yearold children born after ICSI compared to spontaneously conceived children. Hum Reprod. 2006;21(11):2922-2929.
- Auerbach AJ, Oreopoulos P. Generational Accounting and Immigration in the United States. Cambridge, MA: National Bureau of Economic Research; March 1999. NBER Working Paper W7041.
- Schmidt L. Effects of infertility insurance mandates on fertility. J Health Econ. 2007;26(3):431-446.
- Kim CW. Daring population policy [editorial]. Korean Herald. March 2, 2007:3568.
- Birenbaum-Carmeli D. Cheaper than a newcomer: on the social production of IVF policy in Israel. Sociol Health Illn. 2004;26(7):897-924.

